Fat Pad Injury, Fat Pad Impingement & Lateral Conflict Pain in the Knee
If you have sharp, catching pain at the front of your knee – especially when straightening the leg fully or standing for long periods – there is a good chance the infrapatellar fat pad is involved. Fat pad impingement (sometimes called Hoffa's fat pad impingement or lateral conflict pain) is a common but often under-recognised cause of anterior knee pain. I see it frequently in runners, in people who kneel for work, and after knee injury or surgery.
The key to treating it well is understanding why the fat pad is being irritated – not just that it is. That usually means looking at the whole kneecap and how it moves, not just the fat pad itself.
What is the fat pad in the knee?
At the front of the knee, beneath the kneecap (patella) and patellar tendon, sits a soft structure called the infrapatellar fat pad (Hoffa's fat pad). It is richly supplied with nerves and blood vessels, and it:
- Helps cushion the joint
- Fills the space as the knee bends and straightens
- Supports smooth movement of the patellar tendon and kneecap
Because the fat pad is one of the most nerve-rich structures in the knee, even small areas of irritation or pinching can cause surprisingly significant pain.
What is fat pad impingement and lateral conflict pain?
Fat pad impingement occurs when part of the fat pad gets pinched between the femur (thigh bone) and the kneecap or patellar tendon during movement. This can lead to:
- Local inflammation and swelling within the fat pad
- Thickening and scarring over time
- Sharp "catching" pain when the knee is straightened or overloaded
Lateral conflict pain is the most common pattern and affects the outer part of the fat pad and surrounding tissues on the outside of the kneecap. This is often linked to kneecap tracking problems, subtle alignment issues, or overload in specific positions. I find it is one of the most frequently missed diagnoses in anterior knee pain – many patients I see have been told they have "patellofemoral pain" when the fat pad is actually the primary pain generator.
Causes and risk factors
- Overuse or overload – running, jumping, deep squats, repeated lunges
- Direct impact or a fall onto the front of the knee
- Previous knee surgery, particularly around the patellar tendon or kneecap
- Patellofemoral problems – kneecap maltracking, instability, or patellofemoral arthritis
- Hyperextension – habitually "locking back" the knee when standing
- Leg alignment or foot posture that alters front-of-knee loading
Fat pad pain is often part of a wider patellofemoral problem. I always assess the kneecap tracking and the broader mechanics of the leg, because treating the fat pad in isolation without understanding why it is being overloaded usually leads to recurrence.
Symptoms of fat pad impingement and lateral conflict pain
Common symptoms include:
- Sharp pain at the front or front outer side of the knee
- Pinching pain when the knee is fully straight or slightly hyperextended
- Discomfort when standing still with the knees locked back
- Pain with stairs, downhill walking, squats or lunges
- Tenderness if you press either side of the patellar tendon, just below the kneecap
- Swelling or a feeling of fullness at the front of the knee
Symptoms often flare with increased activity, long days on your feet, or exercises that push into end-range extension or deep flexion without good control.
How I diagnose fat pad impingement
The two things I need to establish are: is the fat pad truly the pain source, and what is driving the overload?
Clinical assessment
I take a detailed history – when the pain started, which activities make it worse, whether there has been previous injury or surgery, and what your sport and work demands are. On examination, I check for tenderness around the fat pad, pain on full extension, patellofemoral tracking, limb alignment, and hip and foot mechanics.
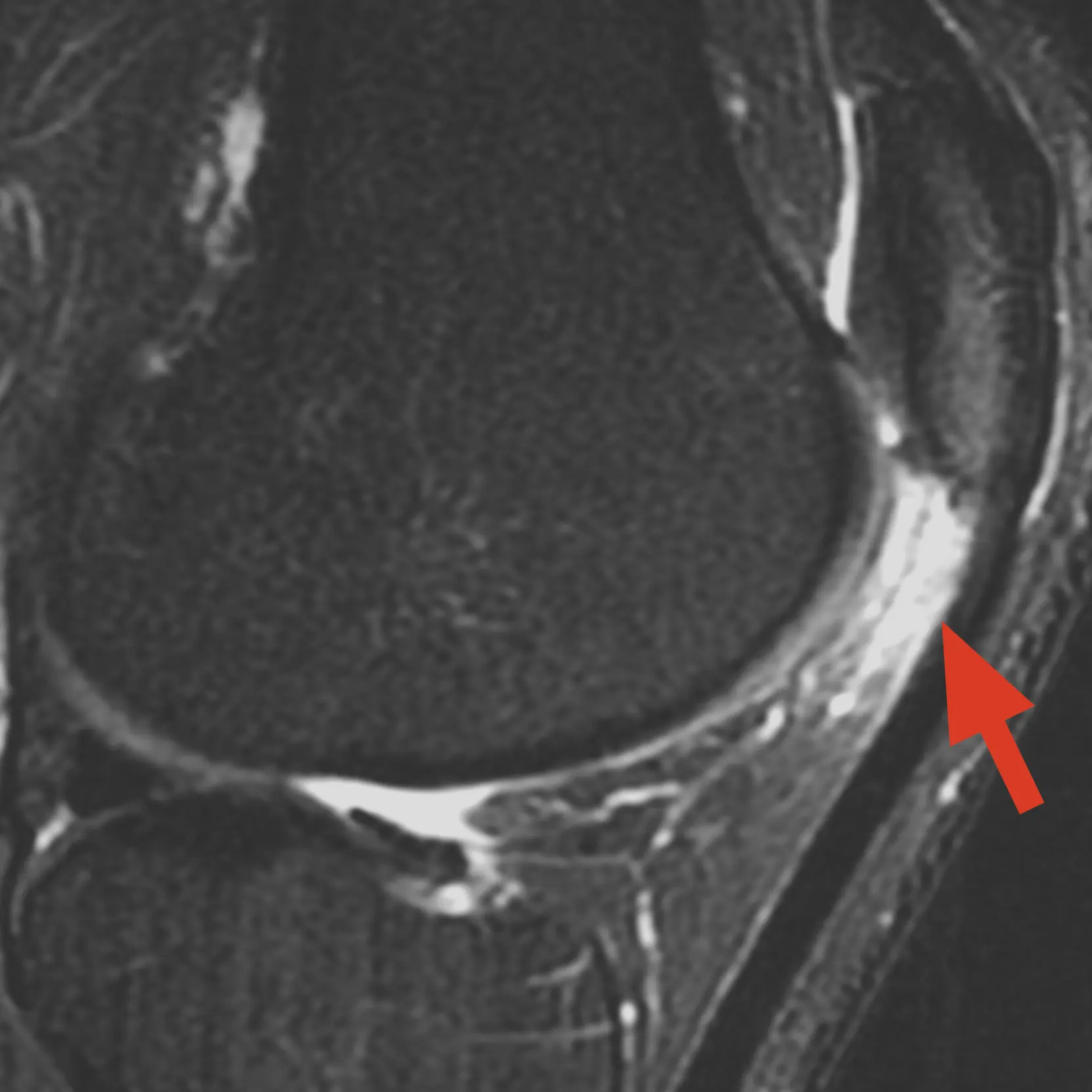
Imaging
- X-rays: to assess bone alignment, kneecap position, and any arthritis
- MRI scan: can show fat pad inflammation, scarring, oedema, and associated issues such as cartilage damage or patellofemoral problems
The aim is to confirm fat pad impingement and to check for other causes of front-of-knee pain, such as patellofemoral cartilage injury, plica, or tendon problems.
Non-surgical treatment (first-line care)
Most patients with fat pad impingement or lateral conflict pain improve with targeted non-surgical treatment. The key is to reduce irritation while improving strength, control, and movement patterns.
Activity modification
- Reduce or temporarily avoid activities that sharply flare symptoms – deep lunges, repeated jumping, hyperextension
- Avoid standing with the knees "locked back"
- Adjust training volume and surface to allow the knee to settle
Specialist physiotherapy
Physiotherapy is central to successful treatment. A good programme typically includes:
- Load management and graded return to activity
- Hip and glute strength to improve leg alignment and control
- Quadriceps and hamstring flexibility and conditioning without provoking impingement
- Balance and proprioception – optimising control of the whole muscular chain
- Movement retraining (landing, squatting, stair technique)
Bracing, taping and orthotics
- Taping or bracing to help offload the fat pad or improve kneecap tracking
- Footwear and orthotics to modify load, where relevant
Injections
A carefully placed injection can help reduce inflammation and pain, making physiotherapy easier. Options may include image-guided local anaesthetic and steroid around the fat pad, or other injections where there is coexisting osteoarthritis or synovitis. I use injections as part of a broader plan – they are not a stand-alone fix.
When is surgery considered?
Surgery is reserved for patients whose symptoms remain troublesome despite well-managed non-surgical care, and where imaging and examination clearly support fat pad impingement or lateral conflict as the main pain driver.
Tibial Tubercle Osteotomy (TTO) for Fat Pad Impingement
In a small number of cases, fat pad impingement and lateral conflict pain are driven by underlying patellofemoral malalignment or patella alta (a high-riding kneecap). If the kneecap sits too high or tracks too far laterally, the fat pad and surrounding structures can be repeatedly pinched, and symptoms may persist despite excellent physiotherapy and injections.
This is where the diagnosis connects directly to surgical decision-making. Tibial tubercle osteotomy (TTO) repositions the bony attachment of the patellar tendon on the shin bone. By shifting the tibial tubercle, I can:
- Improve kneecap tracking within the groove at the front of the femur
- Reduce lateral conflict where the outer fat pad and soft tissues are being pinched
- Address patella alta by lowering the kneecap to a more normal position
- Redistribute patellofemoral load away from overloaded areas
TTO is not a first-line treatment for fat pad impingement. I consider it only when:
- Comprehensive non-surgical treatment has been followed and symptoms remain limiting
- Imaging and assessment show clear patellofemoral malalignment or patella alta contributing to the problem
- There is a clear biomechanical rationale that realignment will reduce fat pad conflict and long-term overload
The operation is combined with a structured rehabilitation programme focused on controlling swelling, restoring movement, and building strong, well-controlled patellofemoral mechanics. Where appropriate, TTO may be performed alongside other patellofemoral procedures (such as MPFL reconstruction or cartilage surgery) as part of a wider plan to address front-of-knee pain and instability.
Fat pad pain within patellofemoral problems
Fat pad impingement frequently coexists with other patellofemoral conditions:
- Patellofemoral pain
- Kneecap maltracking or tilt
- Patellar instability or dislocation
- Patellofemoral cartilage damage or arthritis
For this reason, I often manage fat pad pain alongside wider patellofemoral assessment and treatment, which may include physiotherapy, taping, bracing, injections, and where the anatomy supports it, kneecap stabilisation or osteotomy procedures.
Recovery and outlook
With accurate diagnosis and a structured plan, many patients experience substantial improvement without surgery. Recovery usually involves:
- Settling inflammation and reducing mechanical irritation
- Improving lower-limb strength, control, and movement patterns
- Gradually restoring walking, sport, and daily activities without sharp "pinching" pain
Where surgery is needed, most patients can expect a period of protected rehabilitation, progressive strengthening, and a structured return to sport or higher-level activity.
Frequently asked questions
Is fat pad impingement the same as patellofemoral pain?
No, but they often overlap. Patellofemoral pain refers more broadly to pain from the kneecap and its joint surfaces. Fat pad impingement is a specific source of pain beneath or around the patellar tendon. Many patients have a combination of both, which is why I assess the whole patellofemoral system rather than focusing on one structure.
Can fat pad impingement heal without surgery?
Yes. Most cases settle with targeted physiotherapy, load management, taping or bracing, and if needed, a carefully placed injection. Surgery is reserved for persistent cases where symptoms remain limiting despite good non-surgical care.
Why does my knee hurt most when it is fully straight?
Full extension or hyperextension pinches the inflamed fat pad between the bones, triggering sharp pain. Avoiding prolonged "locked back" standing and adjusting movement patterns is often one of the first things I recommend.
Can I continue running with fat pad impingement?
Often you will need to modify or temporarily reduce running while the knee settles and strength improves. A phased return-to-run programme is usually planned with your physiotherapist once symptoms are better controlled.
Can I be assessed in Bristol?
Yes. I assess and treat fat pad impingement, lateral conflict pain, and related patellofemoral problems at my clinics in Bristol, with a plan that may include physiotherapy, targeted injections, and where appropriate, keyhole or realignment surgery.
Related knee topics
- Patellofemoral pain and kneecap instability
- Cartilage injury and cartilage repair
- Meniscal tears and meniscal repair
- Knee osteoarthritis
- Knee injections
- Knee osteotomy (realignment surgery)
If you have persistent front-of-knee pain, locking, major swelling, or a recent injury with instability, specialist assessment can help identify the cause.









