MCL Injury (Medial Collateral Ligament Tear) and MCL Surgery
The MCL is the most commonly injured ligament in the knee, and the good news is that most MCL tears heal without surgery. But "most" is not "all" – and the decision about whether yours needs more than bracing and physiotherapy depends on what exactly is torn, where, and what else is going on in the knee.
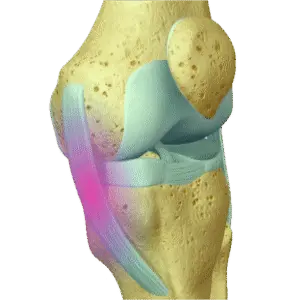
An MCL injury is damage to the medial collateral ligament, the main stabiliser on the inner side of the knee. It resists forces that push the knee inward and also contributes to rotational stability. MCL injuries are common in sport and can range from a mild sprain to a complete tear. Where surgery is needed – either MCL repair or MCL reconstruction – early specialist assessment makes a significant difference to the options available.
What does the MCL do?
The MCL runs along the inner side of the knee, from the thigh bone (femur) to the shin bone (tibia). It:
- Prevents the knee from opening up on the inner side (valgus stress)
- Supports stability during twisting and pivoting movements
- Works alongside other ligaments (including the ACL) to maintain overall knee stability
How MCL injuries happen
MCL injuries typically occur when a force pushes the knee inward:
- A tackle or collision to the outside of the knee
- An awkward landing or twist with the knee collapsing inward
- Skiing or contact sport injuries
- Combined ligament injuries (for example ACL + MCL)
Symptoms of an MCL injury
- Pain and tenderness along the inner side of the knee
- Swelling (often localised, sometimes more widespread)
- Feeling the knee is unstable, especially side-to-side
- Pain when turning, pivoting or changing direction
- Reduced confidence with walking on uneven ground
When to seek urgent assessment
Seek urgent advice if you cannot weight-bear, have a locked knee, major swelling after injury, numbness/weakness in the leg, or if you suspect a multi-ligament injury.
Grading: how severe is the tear?
MCL injuries are commonly described in grades:
- Grade 1: mild sprain – ligament stretched but intact
- Grade 2: partial tear – more pain and some looseness
- Grade 3: complete tear – significant looseness and instability
The grade helps guide treatment, but I also factor in associated injuries, your stability symptoms, and what you need from the knee.
How I assess MCL injuries
Getting the diagnosis right matters because an MCL injury can occur alone or alongside other injuries – especially ACL tears, meniscus damage, or posteromedial corner injuries. I focus on where exactly the tenderness is, how the knee opens on valgus stress testing (both at 30 degrees and in full extension), and whether other ligaments feel lax.
An MRI usually confirms the tear grade, location (femoral side versus tibial side), and associated injuries. X-rays can rule out fractures or bony avulsions. The location of the tear is particularly important – it influences whether repair is feasible and how the ligament is likely to heal.
Non-surgical treatment
Many isolated MCL injuries heal well without surgery because the MCL has a relatively good blood supply compared with ligaments like the ACL.
Non-operative treatment typically involves:
- Short-term activity modification to allow healing
- A brace to protect against inward stress, particularly for grade 2 and 3 tears
- Physiotherapy to restore movement, reduce swelling, and rebuild strength
- Progressive return to sport based on function and stability, not just time
Even for higher-grade tears, I often start with a structured non-surgical approach – particularly when the MCL is expected to heal and stability is improving on re-examination.
When is surgery needed?
I consider surgery when the ligament is unlikely to heal in a stable position, or when persistent medial laxity would compromise function or other reconstructions (such as an ACL graft).
MCL repair
MCL repair means reattaching or repairing the injured ligament. I consider repair when:
- There is a clear avulsion-type injury (ligament pulled off bone) that is suitable for reattachment
- The injury is acute and tissue quality is good
- There is persistent medial laxity despite early management and the tear pattern supports repair, especially alongside ACL reconstruction
- The MCL injury is part of a multiligament injury requiring early stabilisation
MCL reconstruction
MCL reconstruction uses a graft to rebuild the ligament. I recommend reconstruction when:
- There is chronic medial instability (ongoing looseness months after injury)
- The MCL has healed in a lengthened position and the knee remains unstable
- There is combined instability (for example ACL + MCL) where persistent medial laxity would increase stress on an ACL graft
- Tissue quality is poor or the tear pattern is not suitable for repair
- A previous repair or reconstruction has failed and stability remains limiting
In practice, the choice between repair and reconstruction comes down to timing (acute vs chronic), tear location, tissue quality, and whether other ligament injuries are present.
MCL reconstruction graft options
If reconstruction is needed, I rebuild the ligament using graft tissue. The main options are autograft (your own tissue), allograft (donor tissue), or synthetic augmentation. The best choice depends on your injury pattern, goals, and whether other ligaments are being reconstructed at the same time.
Autograft (your own tissue)
Autograft options commonly use tendon tissue from your leg – typically hamstring tendons, depending on your knee and any previous procedures.
Autografts avoid donor tissue and provide robust reconstruction, but they involve harvesting from another area, which can affect early rehabilitation.
Allograft (donor tissue)
Allograft uses sterilised donor tendon. This is particularly useful when:
- Multiple ligaments need reconstruction (multiligament injuries)
- Previous graft harvest limits autograft options
- Avoiding donor-site symptoms (e.g. from hamstring harvest) is preferred
Synthetic augmentation
Synthetic materials can be used to augment a repair or as part of a reconstruction. This is not appropriate for every patient, but it avoids the need for a soft-tissue graft and can provide a robust construct. The trade-off is a small additional risk of local irritation or stiffness.
I discuss which graft option suits your knee and why during the consultation.
What happens during MCL surgery?
The surgical plan depends on whether repair or reconstruction is needed and whether the MCL injury is isolated or part of a multiligament pattern.
- Repair involves reattaching the ligament to bone using anchors or sutures and tightening stretched structures.
- Reconstruction involves placing a graft to restore the MCL's stabilising function, with fixation to the femur and tibia.
In combined injuries, I plan MCL treatment alongside ACL, PCL, or other ligament procedures to restore balanced stability across the knee.
Recovery and rehabilitation
Rehabilitation is essential after MCL injury, whether treated non-surgically or surgically.
Non-surgical recovery
- Focus on reducing swelling, restoring movement, and rebuilding strength
- Bracing for higher-grade tears or when instability symptoms are significant
- Return to sport guided by strength and stability testing, not just time
After MCL repair or reconstruction
- A brace is used initially to protect the healing ligament
- Weight-bearing and range of motion progression are guided by the procedure
- Strengthening and movement retraining progress in stages
- Return to pivoting sport is planned cautiously, based on objective testing and function
Because medial stability influences overall knee mechanics, rehabilitation aims to restore confident side-to-side control and rotational stability.
Risks and considerations
All surgery carries risks. For MCL repair or reconstruction, potential issues include:
- Infection, blood clots, wound healing problems
- Stiffness or prolonged swelling
- Persistent medial laxity or recurrent instability
- Over-tightening (rare) – where the knee feels restrictive if made too tight
- Ongoing pain or difficulty returning to high-demand sport
I discuss these risks alongside expected outcomes and alternatives before we proceed.
Frequently asked questions
Will my MCL tear heal without surgery?
Many isolated MCL injuries heal well with bracing and physiotherapy. I consider surgery when healing is unlikely to restore stable function or when instability persists. It is really important to be seen early – if surgery is needed, doing it in the acute phase is much more straightforward than dealing with a chronically stretched ligament later.
How do you decide between repair and reconstruction?
Repair works best in acute injuries with good tissue quality – especially avulsions where the ligament has pulled cleanly off bone. Reconstruction is more appropriate for chronic instability, poor tissue quality, or when the ligament has healed in a lengthened position. The timing and tear pattern usually make the decision clear.
Do I need surgery if I also have an ACL injury?
Not always. Some MCL injuries heal well enough while the ACL is treated with rehabilitation or reconstruction. However, if the medial side remains lax, it can increase stress on an ACL graft – so I consider combined treatment when the instability pattern suggests it is necessary.
Can I be assessed for an MCL injury in Bristol?
Yes. I see patients with MCL injuries at my clinics in Bristol. Depending on the injury, I offer rehabilitation-led care, repair where the tear pattern supports it, and reconstruction for chronic or complex instability.
Related knee topics
- ACL injury and ACL reconstruction
- Multiligament knee injury and reconstruction
- Meniscal injuries and meniscus surgery
- Knee cartilage injury and cartilage repair
- Return to sport after ligament surgery
If your knee feels unstable after an injury or symptoms are not improving, early assessment helps ensure you get the right treatment at the right time.









